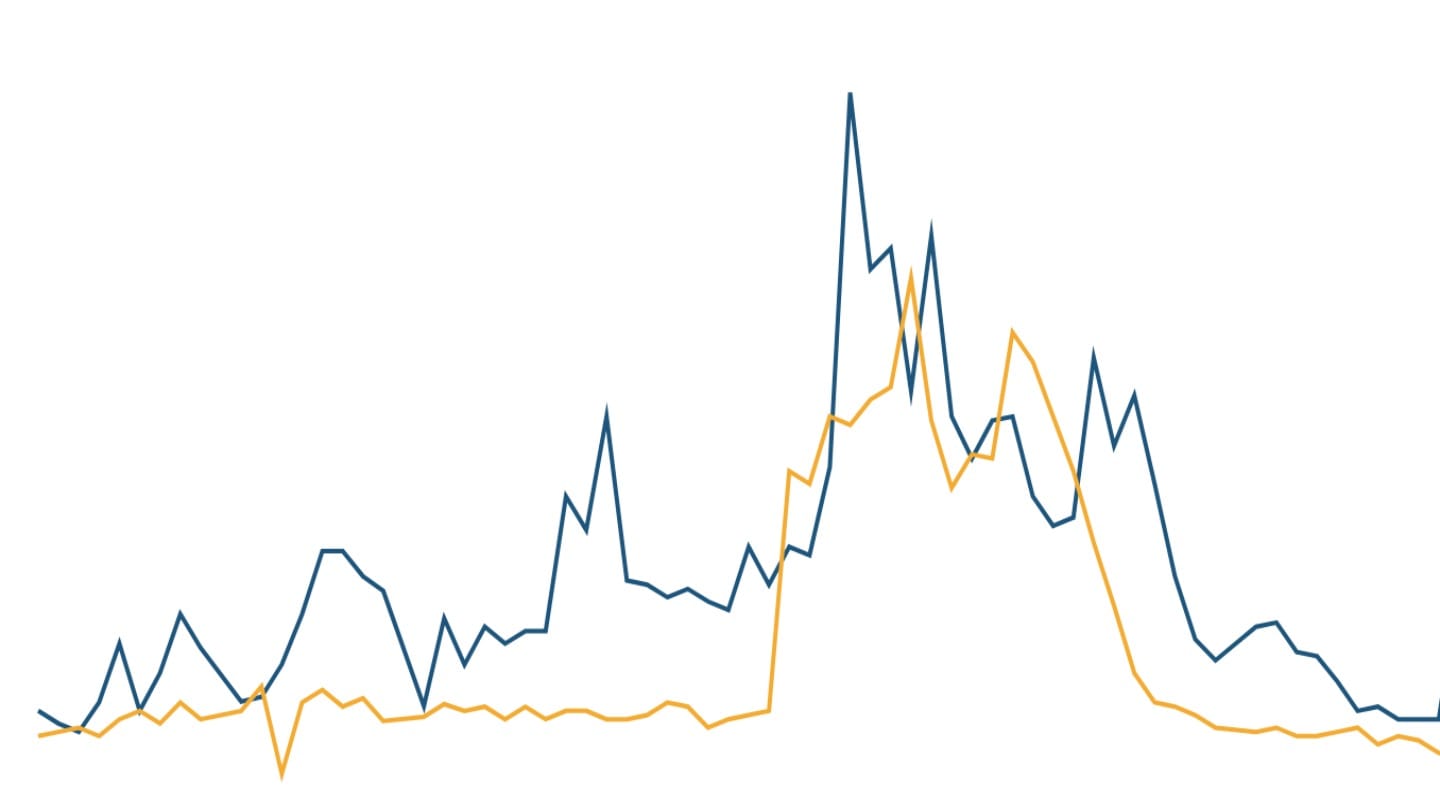
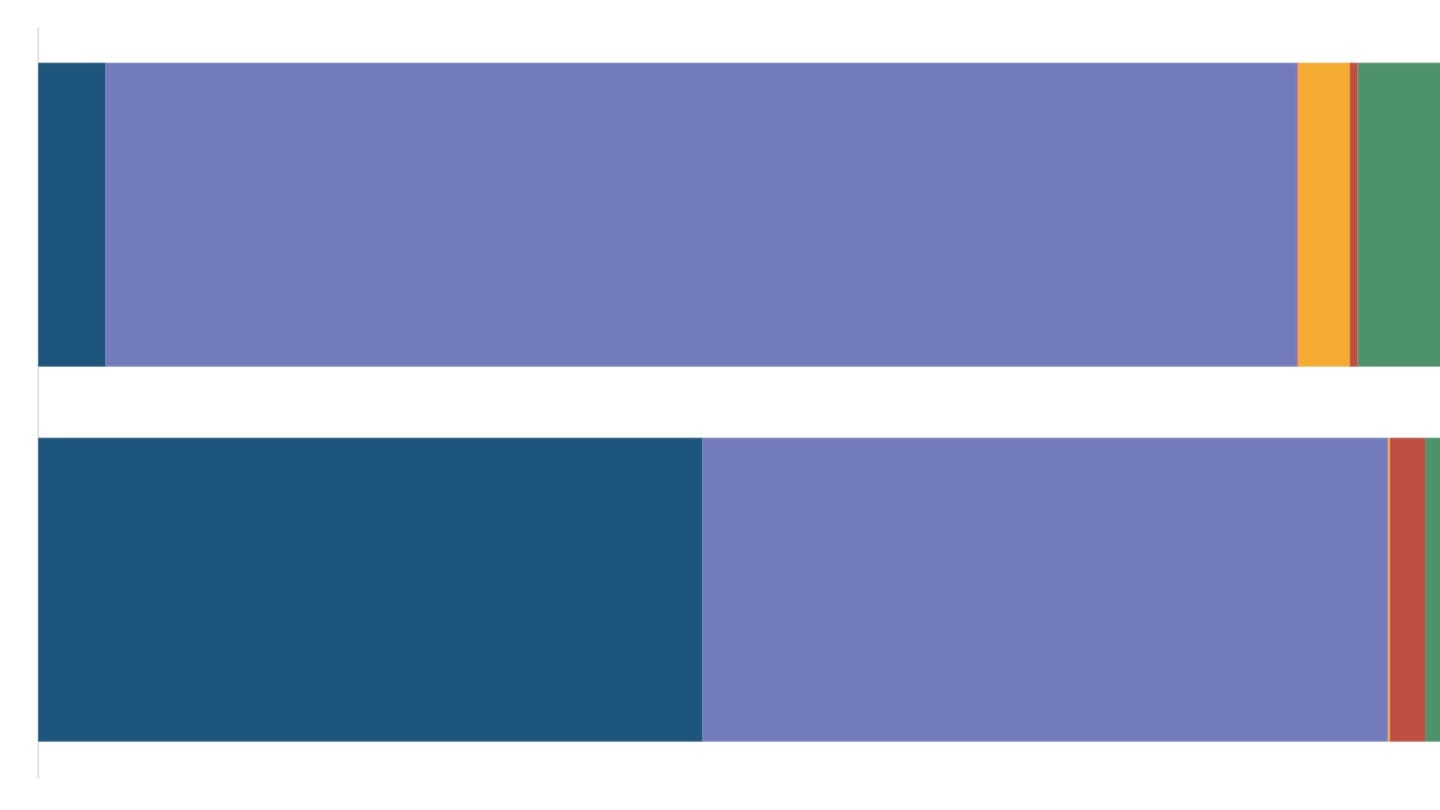Twenty years ago, malaria killed more Indians than diabetes, and diarrhoea killed more people than cancer.
This wasn't unexpected - in 2000, India's per capita income was less than $500, which made it a low income country in the World Bank's classification of countries of the world. Many more people die of infectious or communicable diseases in poorer countries; "When a group - either geographical or social - is at low levels of income with poor nutrition and low levels of access to a clean environment and healthcare, communicable diseases and conditions related to childbirth account for most deaths," I wrote in this early piece for Data For India about the shifting disease environment in India. So it wasn't just India in the position that it was; Pakistan, Bangladesh and Cambodia were all roughly as poor as India was, and roughly as prone to deaths from infectious diseases.
But we've had a big shift in the last twenty years - and so has most of the rest of the world.
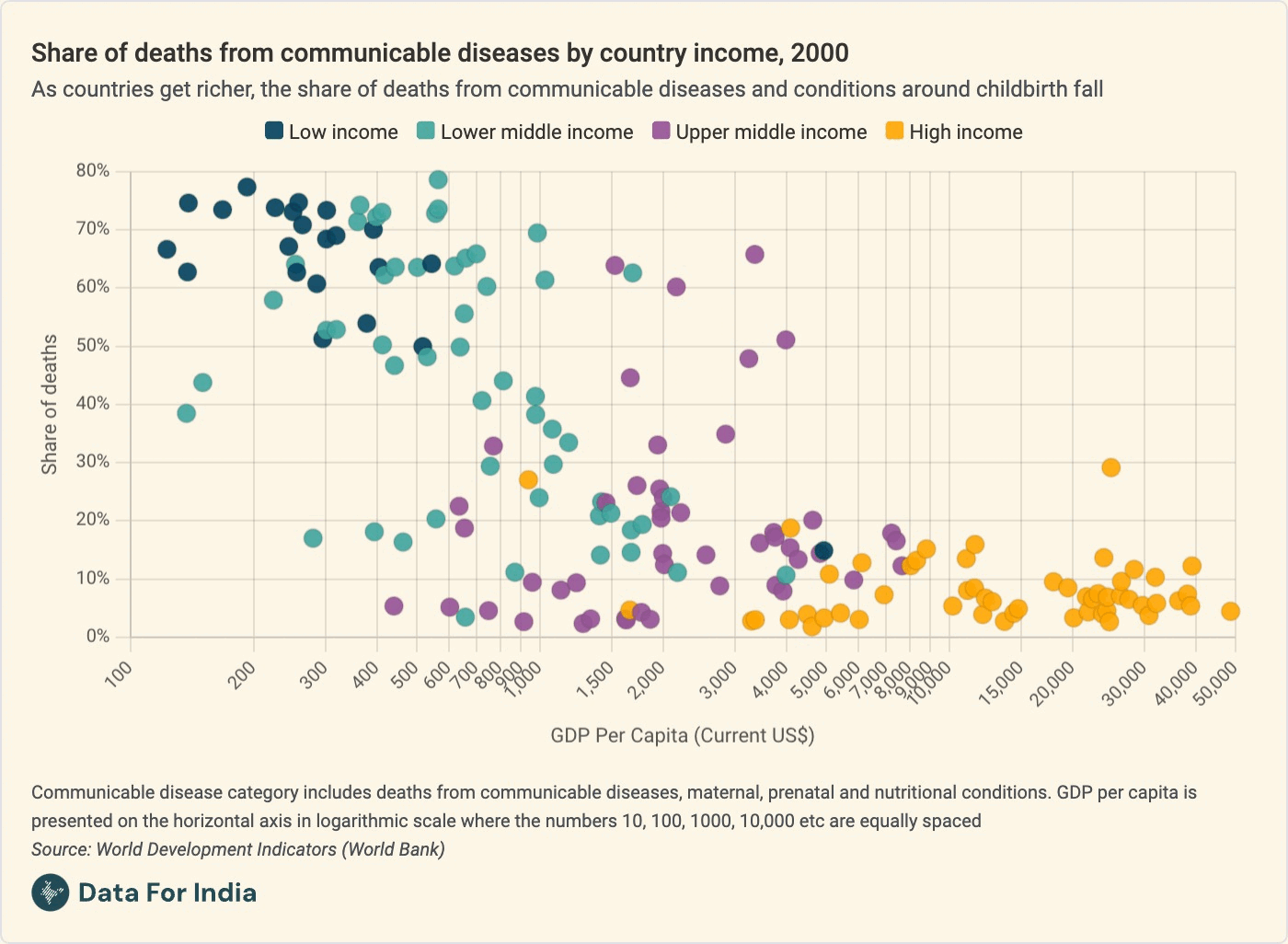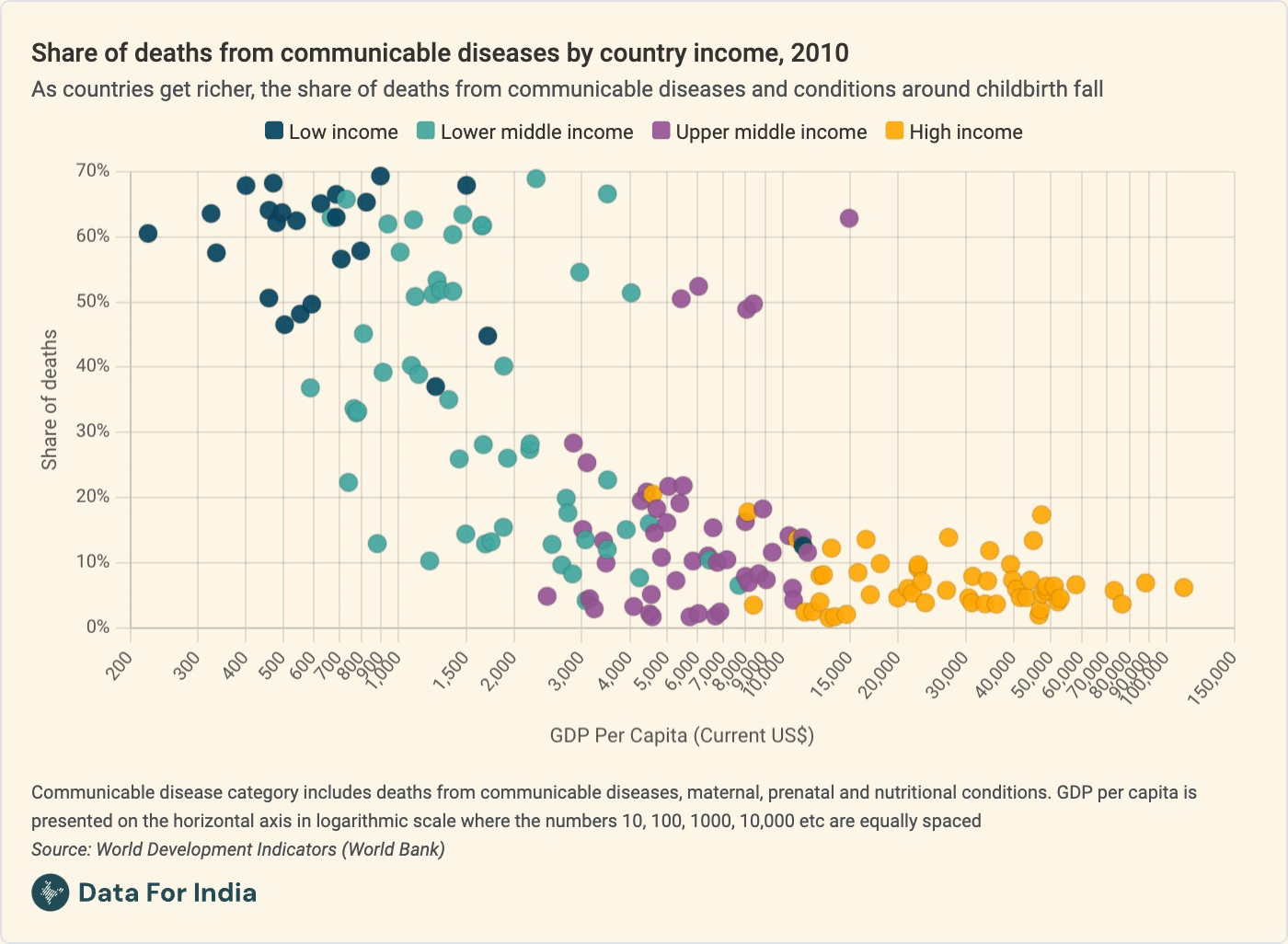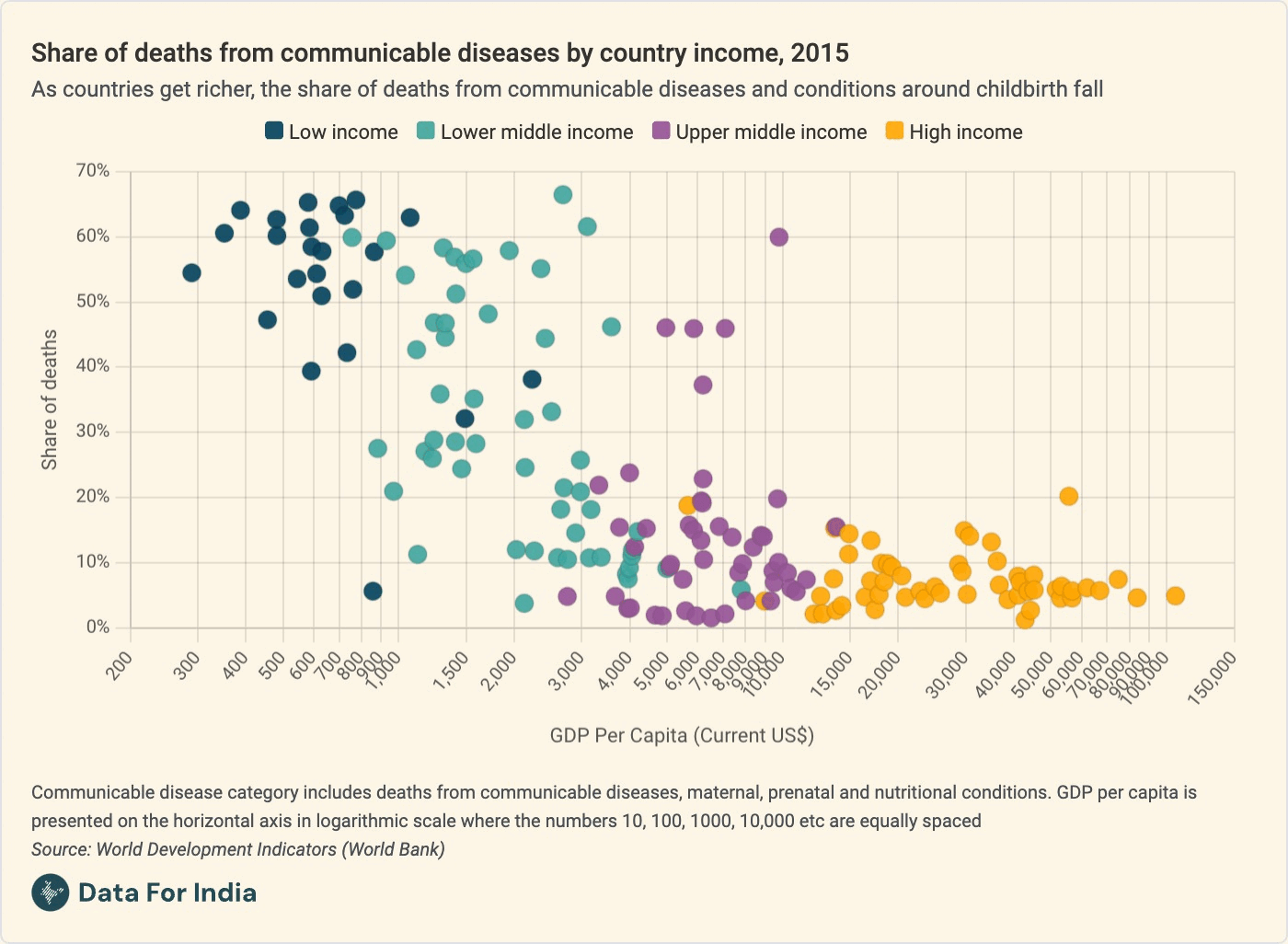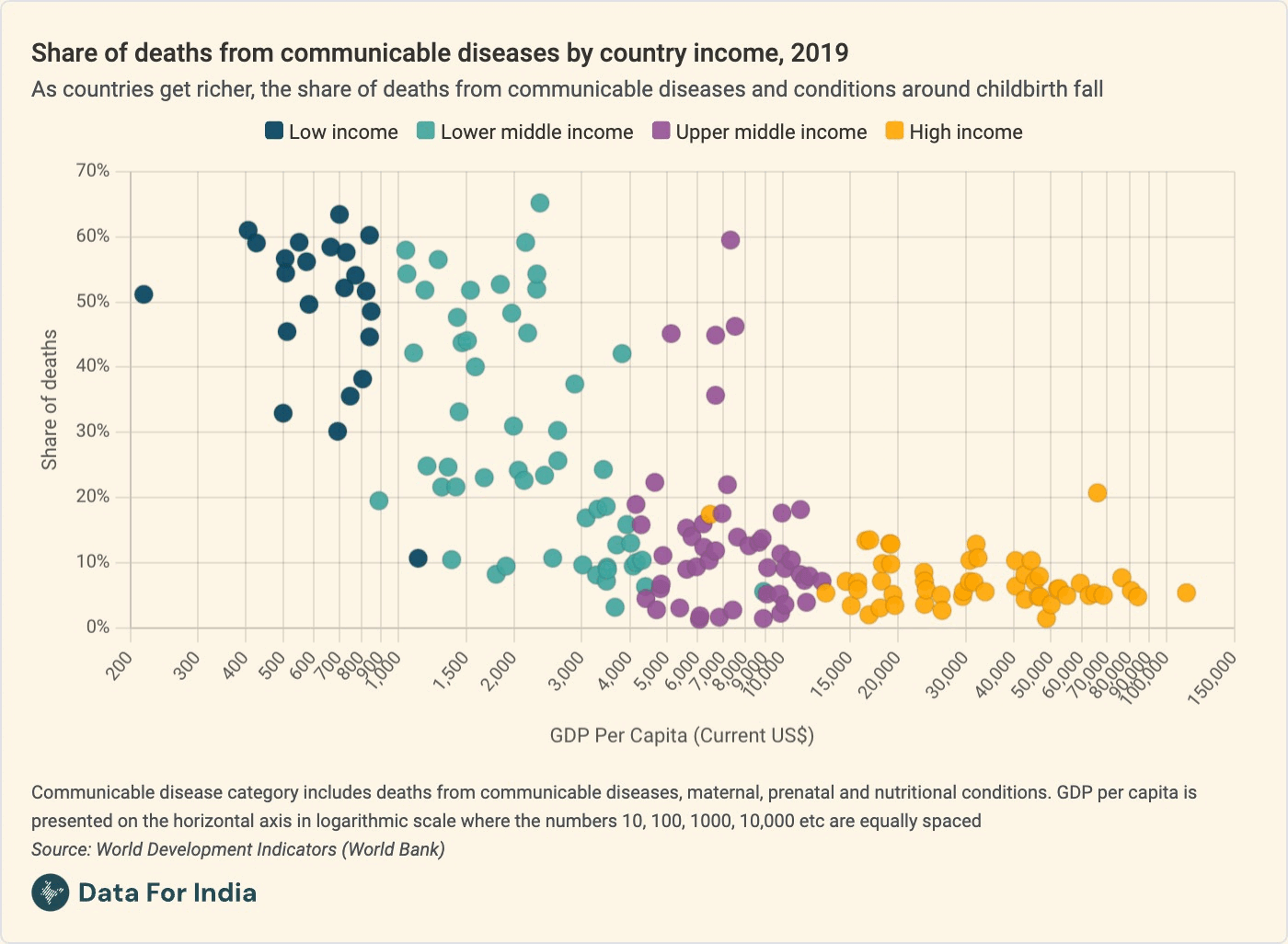
As you'll see in this animated chart that my colleague Pragnya made for us, and as I say in the piece: "As groups get richer and older, deaths from these causes become more preventable and less common. As a result, the relative share of deaths from non-communicable diseases such as heart disease and cancer begins to rise," I wrote in the piece.
We see this in India, where the share of deaths from infectious diseases has halved in the last twenty years, from nearly half of all deaths to a quarter now. Today, cancer kills twice as many people as diarrhoea does, and diabetes kills eight times as many people as malaria does. (For a full list of causes of death by gender and age group, then and now, play around with the explorer at the end of the piece.)
There's good reason to ask why this matters - after all, the total number of annual deaths in India has remained fairly stable (in the region of ten million deaths every year), and is now in fact beginning to rise again. So why should it matter if people are dying of one thing and not another?
For one, deaths from infectious diseases are largely preventable, through better nutrition, limiting exposure, better medicines and vaccines - these were deaths that should not have occurred if access to healthcare and better living standards had been more widespread. Then there is the fact that infectious diseases disproportionately affect the most vulnerable - the very young and the very poor.
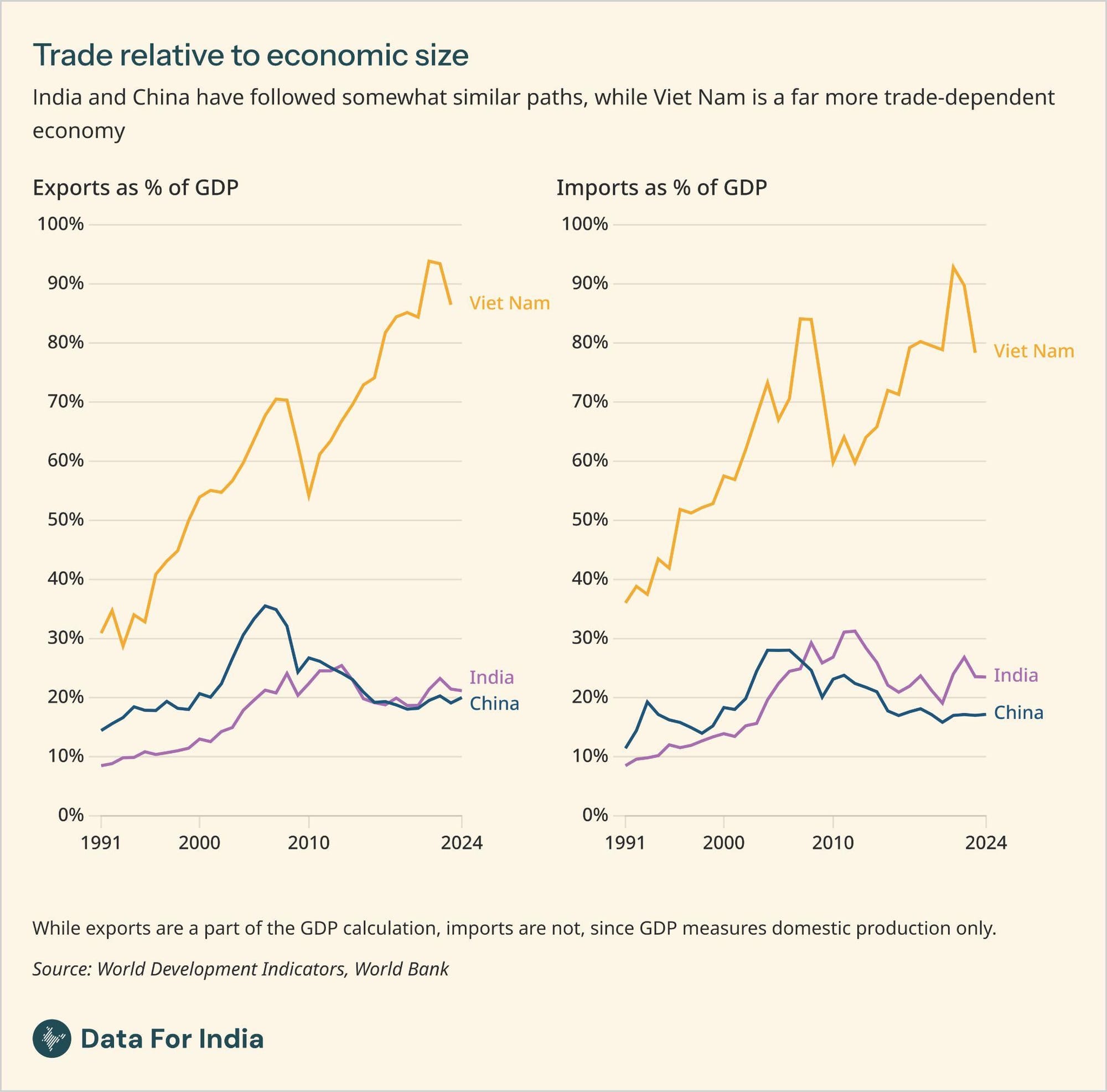
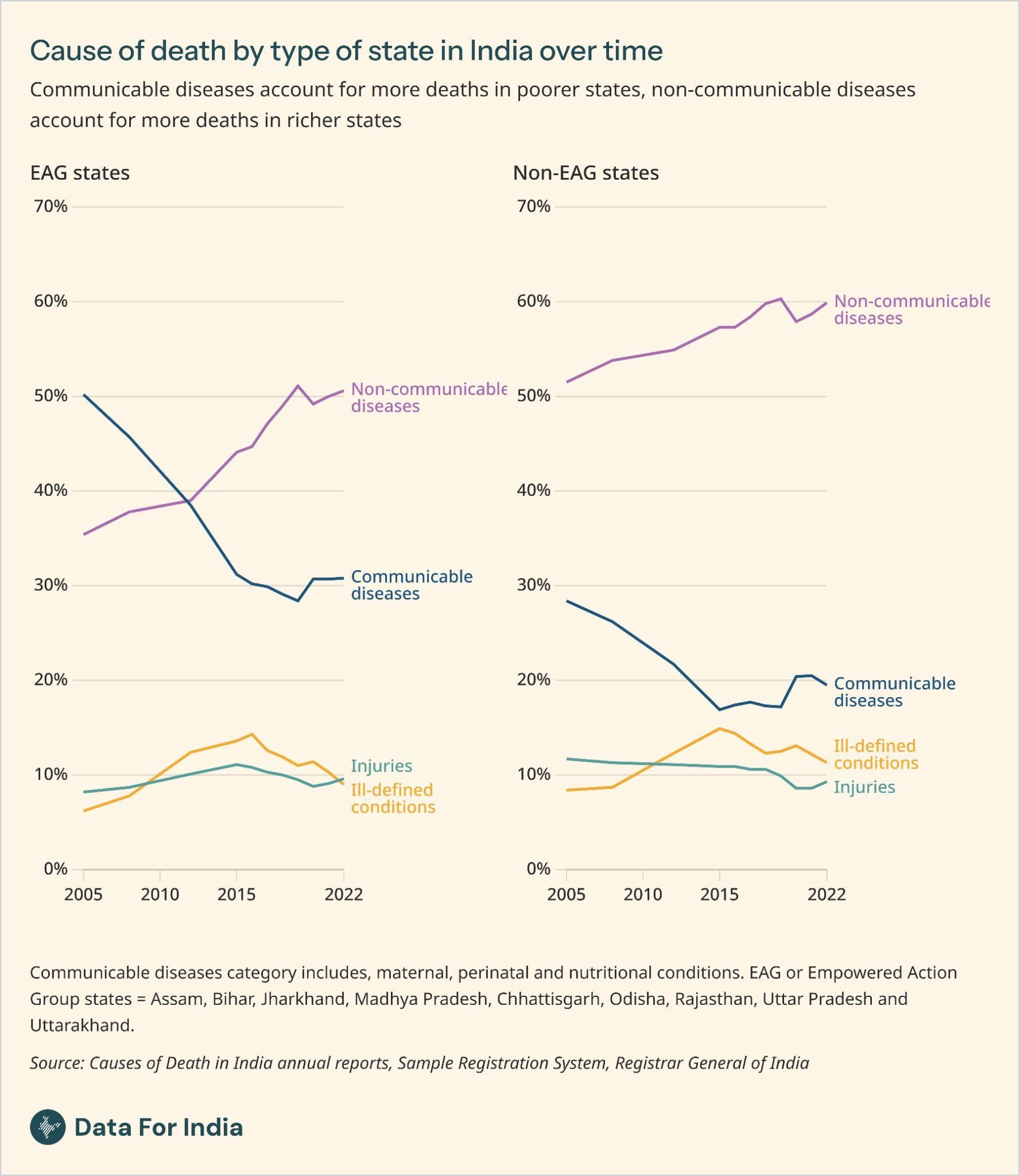
What this does mean, however, is new challenges. The public health discussion about diet and exercise, for instance, has come to India fairly late, but is crucial considering the scale of heart disease in India (it causes nearly 30% of all deaths). It also has an impact on government policies, programmes and funding priorities. It also means different things in different parts of the country - India's poorer states see much more relative mortality from infectious diseases than the richer states.
Demographers, economists and public health specialists the world over will tell you that what's happening in India is exactly what theory and history tell you to expect - it's even got a name, the "epidemiological transition". That doesn't make it any less startling to see and to experience, or any less challenging to grapple with as a country - and it's this week's big shift.